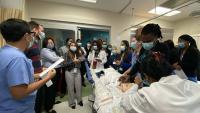
Pediatrics Residency Program
Our educational program is designed for residents to gain the fundamental knowledge and expertise to become the best pediatricians possible, and from there to pursue their individual giftedness, whether that be general pediatrics or subspecialty practice. We challenge residents to become leaders and agents of change in their individual career paths as well as true child advocates.
Mission
The mission of the Pediatrics residency program at Harlem Hospital Center is to train medical graduates, to become full-fledged pediatrician with commitment to providing care, that is culturally sensitive to children of all social background and be children’s advocate. The educational focus is community health with training in sub specialties through affiliation with university based hospital.
This aligns with the mission statement of the Harlem Hospital Center: NYC Health + Hospitals/Harlem is committed to improving the health of the Village of Harlem and providing culturally competent, compassionate, quality care to our patients in a safe environment.
Aims
The program aims to:
- Provide an environment that encourages residents to develop the skills of scholarship, inquiry and critical thinking
- Promote the growth of residents to acquire the knowledge, skills and attitude in primary and sub specialty areas
- Deliver culturally competent care in the patient’s primary language
- Train residents to utilize basic understanding of quality improvement, patient safety, and research principles
Goals
The program’s goals are to:
- Train residents to provide care to patients of all backgrounds
- Develop healthy communities addressing the social determinants of health
- Prepare residents for subspecialty training, based on their professional career choices
Values
- Integrity
- Compassion
- Accountability
- Respect
- Excellence
About Harlem Hospital
NYC Health + Hospitals/Harlem provides a wide range of medical, surgical, diagnostic, therapeutic, and family support services to the residents of Central Harlem, West Harlem, Washington Heights, and Inwood.
We anticipated today’s health issues long ago, instituting wellness programs, measuring patient satisfaction, and implementing quality review programs to assure that our patients receive the highest quality health care.
The hospital is a 272-bed acute care facility and a Level I Trauma Center, designated Stroke Center, Bariatric Center of Excellence, Breast Imaging Center of Excellence, Sexual Assault Forensic Center of Excellence, AIDS Designated Center, National Association of Public Hospitals Safety Net Hospital and Level III Designated National Committee for Quality Assurance Patient Centered Medical Home; Level III Neonatal Intensive Care Unit, an Area Wide Burn Center and the World Health Organization’s UNICEF Designated Baby-Friendly Hospital. The hospital is also designated as a Heart Care Station by the American Heart Association and participates in the 911 Receiving Hospitals Advisory Committee.
NYC Health + Hospitals/Harlem is the largest hospital in Central Harlem, capable of treating the most seriously ill. The hospital provides over 90 specialized ambulatory care services, including same-day surgery in our Aubrey S. Maynard Ambulatory Surgery Unit, behavioral services, community substance abuse treatment, dentistry, and oral surgery.